Mental health: Psychotherapy and Drugs Help Different Brain Areas
Camilla Nord reports that psychotherapy changed aspects of the brain’s prefrontal cortex whereas medications affected the amygdalaWhether to treat mental health issues with psychotherapy or drugs has sometimes led to pitting one against the other. For example, as Cambridge neuroscientist Camilla Nord has noted, in a report that no longer seems to be online, the British Psychological Society’s Division of Clinical Psychology stated in 2016 that “There is no firm evidence that mental distress is primarily caused by biochemical imbalances, genes, or something going wrong in the brain …” Rather, the Society cited childhood trauma, abuse, and poverty as causes, to be remedied by political and social change. Other studies (here is a systematic review) found the same thing.
Nord responds that mental disorders are brain disorders. However, she does not resort to simplistic claims that the mind is simply “what the brain does”; she comes up with something rather interesting instead: Psychotherapy and drugs affect two different areas of the brain.
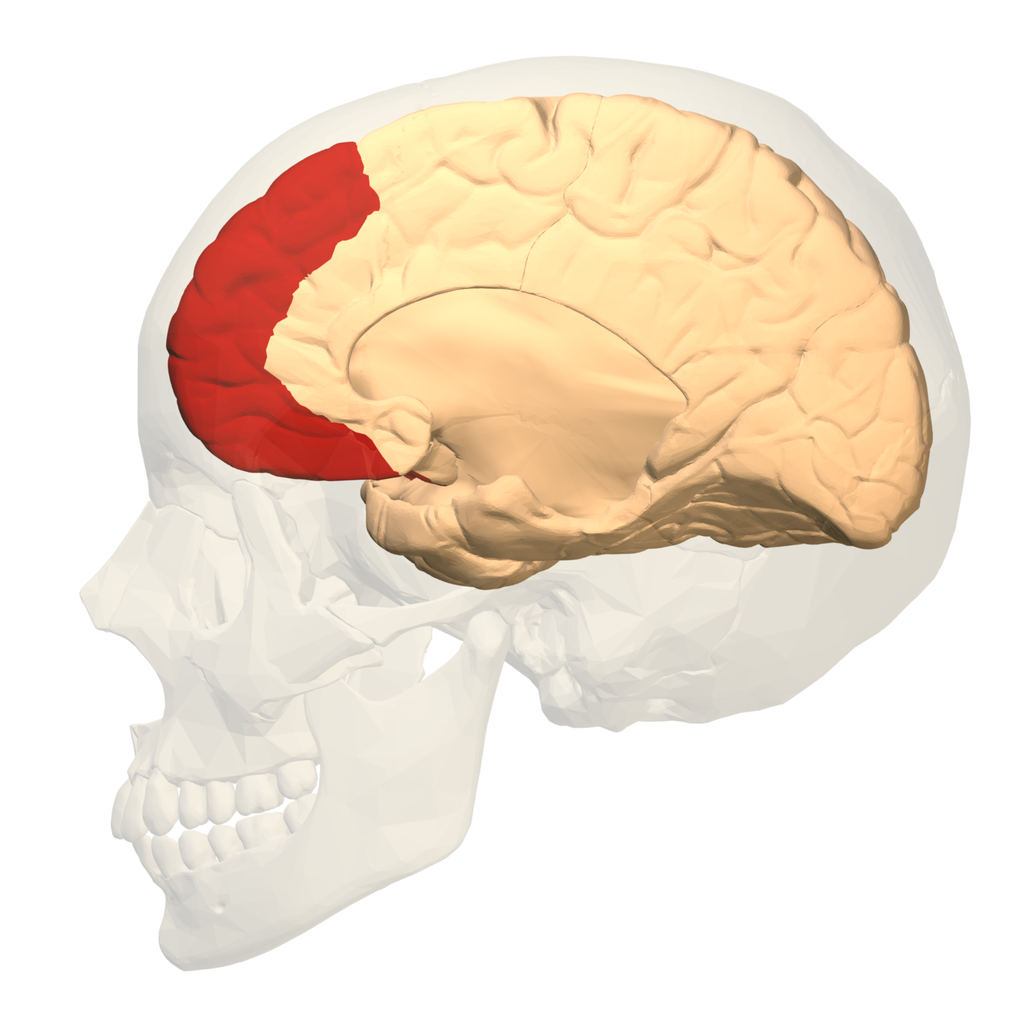
Database Center for Life Science(DBCLS)[2]. –
Polygon data are from BodyParts3D[1], CC BY-SA 2.1 jp
She and colleagues reviewed 24 antidepressant trials and 19 cognitive therapy trials in an open-access paper and here is what they found:
The results were striking – there was no overlap between the brain changes from antidepressant medication and those from psychological therapy. Instead, psychological therapy specifically changed brain activation in the medial prefrontal cortex, a region involved in attention and awareness of your emotional state, whereas antidepressant medication specifically changed activation in the amygdala, which is more directly implicated in generating emotional states.
Camilla Nord, “Mental disorders are brain disorders – here’s why that matters” at Psyche (July 20, 2021)
But, significantly, the different regions were found to work together:
Although medication and therapy affected anatomically distinct regions, these regions are functionally related. In a separate analysis involving data from a large group of participants exposed to emotional stimuli in a brain scanner, we found that both regions significantly overlapped with the brain’s so-called ‘affect network’. This network is made up of interconnected regions in the brain that work together during various emotional or feeling states (angry, happy, sad, and so on). In other words, antidepressant medication and psychological therapy act on different parts of the same functional brain network.
Camilla Nord, “Mental disorders are brain disorders – here’s why that matters” at Psyche (July 20, 2021)
Their work suggested that psychological therapy affects the brain regions that focus conscious attention on our feelings, which is more or less what psychotherapy is designed to do. Antidepressants affect the region of the brain that experiences the feelings — which means that the feelings themselves may change.
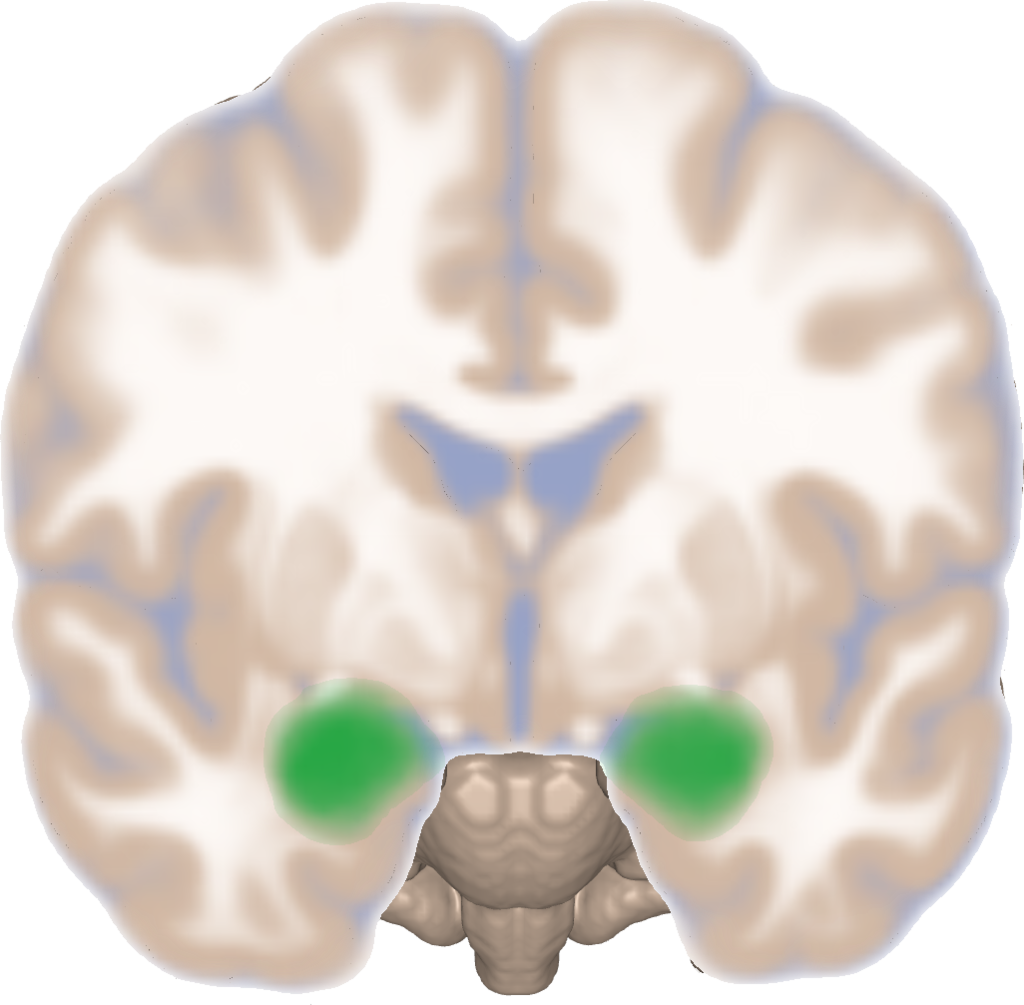
– Own work, CC BY-SA 4.0
If her team is right, the conflict — psychotherapy/social change vs. medication — is misguided. These interventions do different things and can work together. Nord concludes, “These findings have important implications for treatment, implying that the two treatment modalities could work additively; that is, they could be more effective in combination (supporting this, other work has shown that medication and psychological therapy treat depression better in combination than alone).”
But that’s not a complete answer. For some patients, she found, the combined method didn’t work either. Clearly there are other factors at work. One interesting finding was that patients who showed a high level of activity in the prefrontal cortex tended to respond best to treatment.
Nord’s ultimate goal is a much more individualized approach to treatment, based on more detailed information about a given patient’s problems. With luck, that will put some controversies to rest, in the sense that each party is speaking from experience about one aspect of a complex situation and individuals experience different aspects of it in different ways.
You may also wish to read: Neuroscientist: Spirituality helps health directly and indirectly. Andrew Newberg has spent thirty years studying the effects of spirituality using the techniques of neuroscience. Neurotheology, the intersection of neuroscience and spirituality, validates spirituality that is taken seriously enough to change values and lifestyle.
